The Tiniest Patients: Fetal Surgery Delivers Big Results

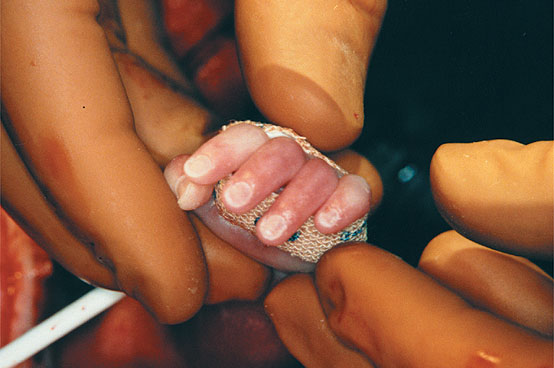
On Nov. 7, 2006, Mary Kelly went for a routine pregnancy ultrasound. Three days later, she and her unborn daughter had become pioneers.
Kelly and her daughter, Addison, now 5 years old, were the second mother and child to undergo a fetal surgery procedure where doctors removed a tumor between the heart and lungs that was causing heart failure and fetal hydrops — a condition where Addison was taking on so much fluid that she would not likely survive.
Over those three days, Kelly underwent tests and met with doctors to discuss her options. With her pregnancy only 26 weeks along, those options included monitoring the pregnancy and waiting, or inducing labor — and in both of those cases, the baby would likely die.
Kelly and her husband opted for a third choice, fetal surgery, which gave their daughter a 50 percent chance of surviving. The surgeons planned to place the fetus back in Kelly's uterus, to allow her to develop for 10 more weeks before delivery, Kelly said.
"But that's not how it went," Kelly said.
While the surgery was successful, a few days later, Mary Kelly went into preterm labor. Addison Hope Kelly was born almost three months premature.
Although Addison faced a multitude of challenges in her young life, and did not even come home from the hospital until she was almost a year old, she will begin kindergarten this fall.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"You look at her, and you would not know she went through any of this," Mary Kelly told MyHealthNewsDaily. Addison needs ongoing observation and requires a machine to ensure she keeps breathing at night, but she has "nothing terrible, which is truly amazing," Kelly said.
Addison's survival and the challenges she has faced represent both the promise of fetal surgery, and the ways it has to go.
The tiniest patients
The first ever open-fetal surgery was performed in 1981, at the University of California, San Francisco (UCSF), to correct an obstructed bladder.
Today, about 150 fetal surgeries are performed yearly at The Children's Hospital of Philadelphia (CHOP), where Kelly was treated and which has the largest volume of these surgeries in the nation, said Dr. Scott Adzick, the surgeon-in-chief.
Adzick was among the researchers who contributed to the development of fetal surgery in the 1980s, [JB1] Since then, fetal surgeons have removed tumors, repaired holes in the diaphragm affecting lung development and treated conditions that threaten twin pregnancies.
"The most successful surgeries have had to do with treatment of twins that share blood through a common placenta in an uneven fashion," said Dr. Ruben Quintero, director of the Fetal Therapy Center at Jackson Memorial Hospital in Florida.
Quintero performs only minimally invasive, endoscopic surgeries, and has developed techniques for the procedures, which involve making a quarter-inch incision while a woman is typically under local anesthesia. These procedures reduce the risks of open procedures, which are more likely to bring infections, and the side effects of general anesthesia, which can include nausea, vomiting and not waking up.
Because of these risks, there is a limit to when fetal surgery should be done.
"The surgeries that are done in utero are justified only when the life of the fetus is at risk if surgery is not undertaken, or where severe damage to the fetus can occur if surgery is not undertaken," Quintero said.
He noted, however, that it can also be justified for conditions that carry serious or long-term health consequences, such as the surgeries some centers perform to treat spina bifida, a condition where the spine is left partly exposed.
"Although [spina bifida] typically is not a lethal condition, it may result in significant complications and surgeries after birth," he said.
Last year Adzick, along with colleagues at UCSF and Vanderbilt University, published a study that compared repairing myelomeningocele — the most severe form of spina bifida — while the babies were in the womb, to the traditional approach of repairing after birth.
While the results showed that mothers and children faced risks from the surgery, the trial was halted early because it overwhelmingly showed that fetal surgery produced better outcomes than repair after birth.
The future of fetal surgery
Efforts under way in fetal surgery involve using less invasive or earlier treatments. One hope is that procedures done today for fetuses who are twentysome weeks old could be done sooner, with greater benefit.
Dr. Alan Flake, director of CHOP’s Center for Fetal Research, is working with stem cells from adult bone marrow to develop a treatment for the blood disorder sickle-cell anemia that could be administered 12 to 14 weeks into pregnancy. Clinical trials of the therapy should begin in a year or two.
In the longer term, Adzick said, researchers are looking at treating other single-gene disorders that can be diagnosed early in pregnancy.
Finally, Adzick said more work is being done for spina bifida. A tissue-engineering technique could be used to protect the spinal cord opening, essentially working as a "band-aid" early on in pregnancy, with repair being done after birth.
But that research needs more rigorous lab testing before being applied to patients.
While fetal surgery has had some dramatic successes, it is not without risks, which can include infection from the surgery, preterm birth or death for the mother or fetus.
That's why part of all lines of fetal surgery research include asking, "Can that be done with tissue engineering, can that be done in some other way that’s not a fetal surgery?" said Lori Howell, executive director of CHOP's Center for Fetal Diagnosis and Treatment.
When fetal surgeries began, Howell said, other physicians were skeptical that opening up a pregnant woman to operate on the baby was necessary.
With the improvements coming in the field, the hope is that someday, many of the operations needed today won't be.
Pass it on: Doctors are looking to use fetal surgery to treat an increasing number of conditions, but the surgery remains risky.
This story was provided by MyHealthNewsDaily, a sister site to LiveScience. Follow MyHealthNewsDaily on Twitter @MyHealth_MHND. Find us on Facebook.


 Live Science Plus
Live Science Plus





