Sneaky Parasite Filmed While Infecting Blood Cells
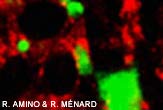
Treating malaria and other diseases caused by parasites requires a good understanding of the parasite. A new video of the malaria parasite at work should help researchers develop better treatments.
The malaria parasites, Plasmodium falciparum and its three relatives, have dodged the human immune system for centuries. The disease is transmitted by mosquitoes and kills more than a million people every year.
Scientists know that the parasite first infects the liver and then somehow gets into the bloodstream, where it causes red blood cells to rupture. It is during this stage of the disease that the classic symptoms—high fever and chills—occur.
A paradox
In the liver, the parasite takes the form of a merozoite, one of its lifecycle stages. Studies have shown that liver's immune cells gobble up free-moving merozoites.
"This was a paradox," explained Robert Menard, a researcher at the Howard Hughes Medical Institute. "We could not understand how the rate of infection could be so successful."
By tracking malaria infections in live mice, Menard and his colleagues discovered a sneaky trick. After infecting the liver, the parasite wraps itself in dead liver cells, called merosomes, to cloak and transport itself back into the bloodstream, where it can do further harm. [VIDEO]
Get the world’s most fascinating discoveries delivered straight to your inbox.
Since the biology of mice is similar to that of humans, the researchers hope the new insight will lead to improved methods for warding off the disease.
Trojan Horse
The scheme is reminiscent of those ancient Greeks who hid in the hollow horse to sneak into Troy.
"The parasite has evolved this complex structure. The best image to describe it is the Trojan Horse, because it both transports the parasites and camouflages them," Menard said.
The parasite has evolved another neat trick. It releases cloaking chemicals while inside the dead liver cell that prevent the cell from broadcasting its own death signal, which would normally be the call for immune cells to seek and ingest it.
The results were reported Aug. 3 in the online version of the journal Science. Volker Heussler at the Bernhard-Nocht Institute for Tropical Medicine in Hamburg, Germany and Rogerio Amino, at the Institut Pasteur in Paris contributed to the work.
Robert is an independent health and science journalist and writer based in Phoenix, Arizona. He is a former editor-in-chief of Live Science with over 20 years of experience as a reporter and editor. He has worked on websites such as Space.com and Tom's Guide, and is a contributor on Medium, covering how we age and how to optimize the mind and body through time. He has a journalism degree from Humboldt State University in California.
 Live Science Plus
Live Science Plus






