Engineering a New Face After Injury
This Behind the Scenes article was provided to LiveScience in partnership with the National Science Foundation.
Today, surgeons face many limitations when it comes to helping a patient who suffers from a severe craniofacial injury, or an injury pertaining to the skull and the face. Most often a result of cancer or war-related circumstances, the injury is both psychologically and physically damaging.
Will the patient ever recover their appearance? Or more importantly, recover their ability to speak, breathe or eat correctly again?
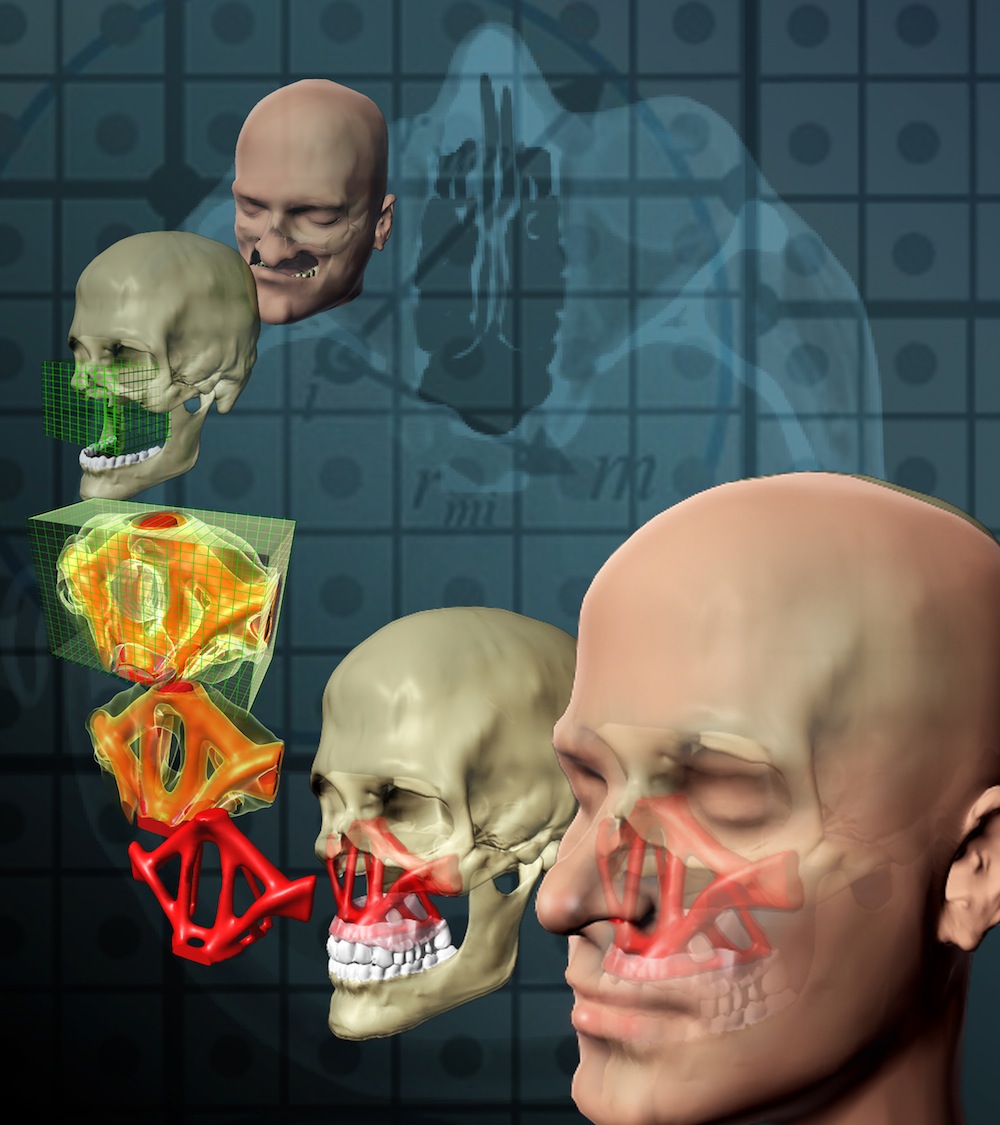
Rebuilding the delicate facial bone structure of an individual is a complicated procedure. The surgeon constructs a facial frame with bone from other parts of the body (called autologous tissue), in order to guarantee the functionality of the specialized organs responsible for vital roles such as breathing, seeing, communicating and eating. Since there are no analogous bone structures to a person's face, the procedure depends on experience and skill. As Glaucio Paulino, program director of Mechanics of Materials at the National Science Foundation, noted, this procedure does not always generate the desired outcome.
"The middle of the face is the most complicated part of the human skeleton," said Paulino. "What makes the reconstruction more complicated is the fact that the bones are small, delicate, highly specialized and located in a region highly susceptible to contamination by bacteria."
Facial bones are unique and using bone tissue extracted from different parts of the body, such as the bones of the forearm, isn't the most effective form of recovery.
"The patient may be improved, but still suffer from significant deformity," said Paulino.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Mathematical medicine
In contrast, topological optimization is a feasible alternative to make such a recovery possible.
Topological optimization isn't native to the surgery room — it's a mathematical method that uses given loads, the applied force on an area, and boundary conditions or spatial limits, to optimize a specific structure's layout. Imagine a building grid in which you can determine where there should be material and where there shouldn't. Moreover, you can express loads and supports that would affect certain parts of this block of material. Your final result is an optimized structure that fits your established constraints.
This mathematical method is successfully used to engineer spaceships and airplanes. The Airbus 380 wing, for example, was designed with topological optimization. Today, extensive research is underway to apply topological optimization to the engineering of future high-rise buildings. Paulino is responsible for some of the recent advances in this field.
Together with Alok Sutradhar and Michael Miller, from the Ohio State University Medical Center and Tam Nguyen, from the Department of Civil and Environmental Engineering at the University of Illinois, Paulino is studying how to bring topological optimization to the surgery room. With the recent advances in tissue engineering, Paulino believes that the method can be used to construct patient specific bone frames.
"The key idea is to have a technique that is tailored for the specific patient. It's not one formula that fits all. People are different, therefore you cannot have one solution for all patients," said Paulino.
Engineering a face
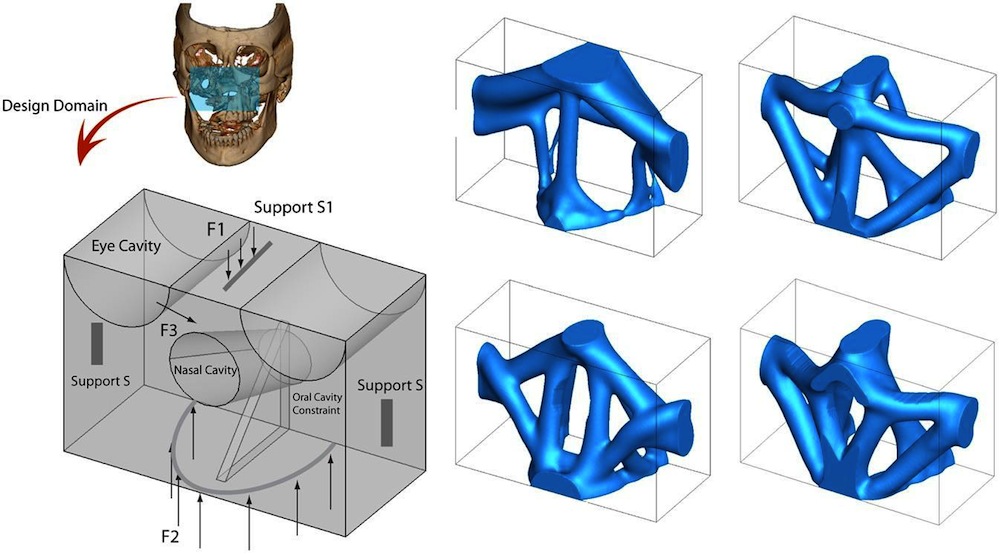
In an experiment, researchers explored the creation of a three-dimensional structure for a patient with severe gunshot injury. After selecting a design domain from the craniofacial skeleton, supports, loads and cavity constraints (areas with no bone, such as eye cavities) were applied. Topological optimization generated many possible structures to fit the patient-specific requirements.
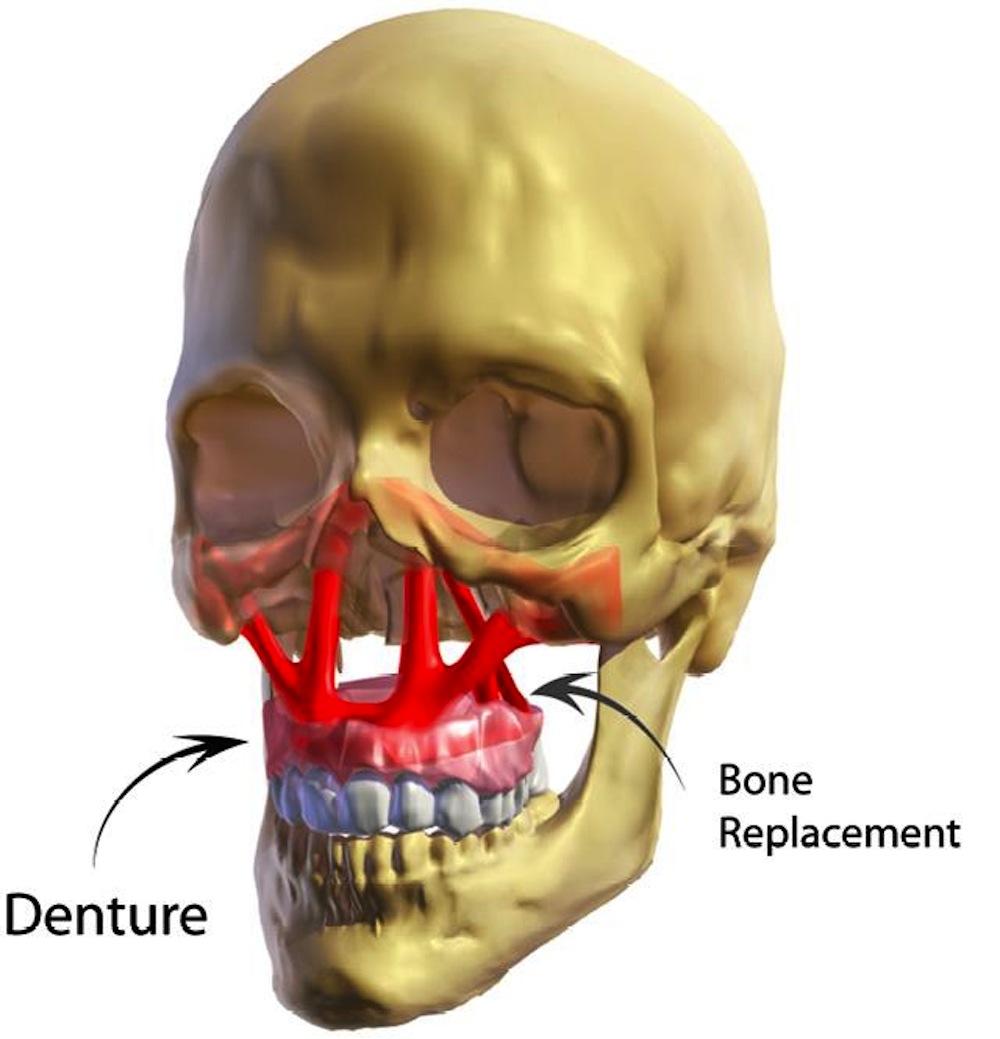
Watch this video to see the process of creating a structure for a patient with severe gunshot injury using topological optimization. Although the results did not necessarily resemble the natural bone structure, they would preserve the vital functions of facial organs while providing a safe platform for prosthetics and plastic surgery.
The process will "show surgeons their alternatives before going into the operating room," said Paulino.
At the moment, such structures would be built using titanium, which is light and strong. Unfortunately, titanium may cause infections because it's foreign to the body. With future advances in tissue engineering, however, molding human bone tissue into a structure is a possibility. Researchers are still investigating how to ensure that the bone structure created through this process, a living tissue, will maintain the desired shape after implanted in the patient.
Paulino and his team of researchers hope to continue translating applicable concepts between different fields, such as engineering and medicine, to make innovative discoveries. With the development of tissue engineering and topological optimization, in the future, complete recovery from craniofacial injuries will hopefully be a routine procedure in the surgery room.
Editor's Note: This research was supported by the National Science Foundation (NSF), the federal agency charged with funding basic research and education across all fields of science and engineering. Any opinions, findings, and conclusions or recommendations expressed in this material are those of the author and do not necessarily reflect the views of the National Science Foundation. See the Behind the Scenes Archive.

 Live Science Plus
Live Science Plus






